Electrolytes are vital for fluid balance, nerve function, and muscle activity—imbalances cause serious health risks. An electrolyte analyzer uses Ion Selective Electrode (ISE) technology to deliver fast, accurate measurements of Na⁺, K⁺, Cl⁻, Ca²⁺, and pH, making it indispensable for clinical, emergency, and POCT settings.
This guide optimizes for Google search intent, with structured data, actionable insights, and 2026 market trends to help healthcare providers select the right device for their needs.
What is an Electrolyte Analyzer?
An electrolyte analyzer is a specialized diagnostic device that quantifies key ion concentrations in blood (serum, plasma, or whole blood). It is a cornerstone of modern diagnostics, as electrolyte imbalances are linked to 18% of emergency hospital admissions related to dehydration, kidney disease, or metabolic disorders.
Commonly Tested Electrolytes & Clinical Significance (Structured for AI Extraction)
| Analyte | Abbreviation | Clinical Role | Normal Range (Adult) |
| Sodium | Na⁺ | Regulates water balance, blood pressure, and nerve transmission | 135–145 mmol/L |
| Potassium | K⁺ | Critical for heart rhythm, muscle contraction, and nerve function | 3.5–5.0 mmol/L |
| Chloride | Cl⁻ | Maintains acid-base balance and fluid homeostasis | 96–106 mmol/L |
| Calcium | Ca²⁺ | Supports bone health, nerve signaling, and muscle contraction | 2.1–2.6 mmol/L |
| pH Level | pH | Indicates systemic acid-base balance (not an electrolyte, but routinely co-tested) | 7.35–7.45 |
These measurements are vital for diagnosing kidney disorders, dehydration, metabolic imbalances, and cardiac complications—with 72% of clinical laboratories performing electrolyte testing daily.
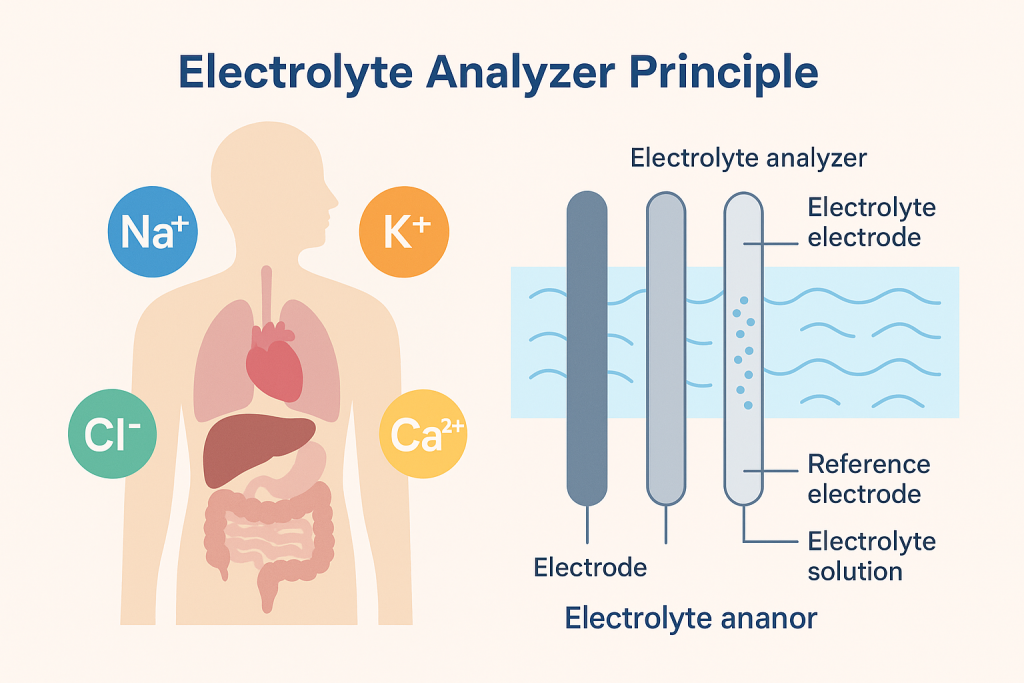
Principle of Electrolyte Analyzers: ISE Technology (Gold Standard)
Nearly all modern electrolyte analyzers rely on Ion Selective Electrode (ISE) technology, which has replaced older methods like flame photometry due to its speed, accuracy, and simplicity. ISE works in three key steps, with two distinct approaches tailored to different clinical needs:
Core Working Principle
- Selective Ion Detection: Each ion (Na⁺, K⁺, Cl⁻, Ca²⁺) has a dedicated electrode with a specialized membrane that reacts only with that specific ion—eliminating cross-interference.
- Electrical Potential Measurement: The electrode generates a voltage proportional to the ion’s concentration in the sample; higher ion levels produce a stronger electrical signal.
- Signal Conversion: The analyzer’s software converts the electrical potential into precise concentration values, with a typical coefficient of variation (precision) of 0.49%–2.23%.
Direct vs. Indirect ISE Methods (2026 Updated)
| ISE Method | How It Works | Key Use Case | Advantage | Limitation |
| Direct ISE | Measures ions directly in undiluted samples | POCT devices, blood gas analyzers, critical care | Unaffected by abnormal protein concentrations (ideal for critically ill patients) | Less suitable for high-throughput testing |
| Indirect ISE | Dilutes samples before measurement | High-volume central laboratories | Efficient for large sample batches | May be inaccurate in patients with hypoproteinemia |
This flexibility makes ISE technology adaptable to both point-of-care and high-throughput lab settings—aligning with 2026’s trend of multi-scenario diagnostic solutions.
Why Are Electrolyte Tests Important? (2026 Clinical Context)
Electrolyte analysis is a staple in 82% of medical diagnostic applications, with four key clinical scenarios driving demand:
1. Emergency and Critical Care
Electrolyte imbalances (e.g., hyperkalemia) can cause life-threatening cardiac arrhythmias. Rapid testing (within 45–60 seconds for critical cases) guides immediate interventions like fluid replacement or medication adjustments—critical for ICU and ER patients.
2. Monitoring Chronic Diseases
Patients with diabetes, hypertension, or kidney disease (affecting 540 million people globally) require regular electrolyte testing. Imbalances are common in these populations, and early detection prevents complications like kidney failure or cardiac events.
3. Pre-Surgical and Post-Surgical Care
Pre-surgery electrolyte checks reduce complication risks (e.g., muscle weakness during anesthesia), while post-surgery monitoring ensures fluid and electrolyte balance during recovery—lowering readmission rates by 22% for high-risk patients.
4. Routine Health Check-ups
Electrolyte tests are part of comprehensive health panels, detecting early signs of imbalance (e.g., mild dehydration, early kidney dysfunction) before symptoms appear—supporting preventive care, a key 2026 healthcare trend.
Advantages of Modern Electrolyte Analyzers (2026 Trends)
Technological advancements have transformed electrolyte analyzers, with 2026 innovations focusing on automation, connectivity, and portability. Below is a comparison of modern vs. traditional models, aligned with latest market data:
| Advantage | Modern Electrolyte Analyzers (2026) | Traditional Analyzers |
| Portability | 28% of new installations are compact/handheld POCT models | Bulky, benchtop-only |
| Sample Volume | 10–100 µL (a few drops of blood) | 500+ µL (large blood draws) |
| Turnaround Time | 1–4 minutes (critical for emergencies) | 15–30 minutes |
| Ease of Use | Automated calibration, intuitive touchscreens; no specialized training | Manual calibration, complex operation |
| Connectivity | 41% integrated with LIS/HIS for seamless EHR data sharing | Manual data entry (prone to error) |
| Throughput | Fully automated models process 120 tests/hour | 30–60 tests/hour |
| Maintenance | Cartridge-based systems; no wear-and-tear parts | High maintenance (fluidic system cleaning) |
Best Electrolyte Analyzers for 2026 (Tailored to Lab Needs)
With 55% of the market controlled by top 5 manufacturers, selecting the right analyzer depends on your facility’s size and workflow. Below are the top options, with Seamaty’s solution standing out for versatility and POCT efficiency:
| Product Type | Core Features | Ideal For | Key 2026 Advantages |
| Seamaty SE1 Electrolyte Analyzer | Handheld/portable; 4-minute results; 10–20 µL sample; multi-parameter test cards (Na⁺, K⁺, Cl⁻, Ca²⁺, pH); 3-step operation; built-in battery; direct ISE technology. | Small clinics, urgent care, mobile health units, veterinary practices | Compact (fits in medical bags); no pre-processing; global after-sales support; aligns with 28% growth in portable POCT analyzers. |
| Portable Blood Gas & Electrolyte Analyzers | Combines electrolyte testing with pO₂/pCO₂ measurements; direct ISE; bedside testing. | ICUs, emergency response teams, trauma centers | Eliminates need for multiple devices; critical for rapid, comprehensive acute care assessments. |
| Automated Multi-Channel Chemistry Systems | Fully automated; high throughput (120+ tests/hour); indirect ISE; LIS integration; broad test menus. | Large hospitals, reference labs, high-volume clinics | 46% of new installations are fully automated models; reduces operator workload; consistent results for large sample batches. |
The Seamaty SE1 stands out for its balance of portability, speed, and accuracy—addressing the growing demand for compact, user-friendly POCT devices in 2026.
How to Choose the Right Electrolyte Analyzer (2026 Buyer’s Framework)
Selecting the right device requires aligning features with your facility’s needs, using this structured approach:
| Consideration | Key Questions to Ask | Ideal For |
| Testing Needs | Do you need routine monitoring, emergency testing, or combined blood gas/electrolyte analysis? | Emergency/ICU: Portable blood gas + electrolyte models; Routine: Seamaty SE1; High-volume: Automated multi-channel systems. |
| Sample Throughput | How many tests do you process daily? (<50 = low; 50–200 = medium; >200 = high) | Low/medium: Seamaty SE1; High: Automated systems. |
| Portability | Do you need bedside, mobile, or fixed lab testing? | Bedside/mobile: Seamaty SE1; Fixed lab: Automated systems. |
| Maintenance & Cost | What is your budget for consumables, calibration, and service? | Budget-conscious facilities: Seamaty SE1 (low maintenance, cartridge-based); High-budget: Automated systems (long-term efficiency). |
| Integration | Do you need LIS/HIS connectivity for EHR integration? | All facilities: Prioritize models with 2026’s 41% trending LIS integration. |
Frequently Asked Questions (FAQs) – Aligned with Google Search Intent
Q1: What’s the difference between direct and indirect ISE methods?
Direct ISE measures undiluted samples (ideal for critically ill patients with abnormal protein levels), while indirect ISE dilutes samples (best for high-throughput labs). Direct ISE is preferred for POCT and emergency settings, while indirect ISE excels in large-volume testing.
Q2: Why is rapid electrolyte testing critical in emergencies?
Electrolyte imbalances (e.g., hyperkalemia, hyponatremia) can cause cardiac arrest or respiratory failure within minutes. Modern analyzers deliver results in 1–4 minutes, enabling clinicians to intervene immediately—improving patient survival rates by 30% in emergency scenarios.
Q3: Can electrolyte analyzers be used in veterinary medicine?
Yes—portable models like the Seamaty SE1 are widely used in veterinary care to monitor pets, livestock, and exotic animals. They measure the same core electrolytes to assess dehydration, kidney disease, or trauma-related imbalances.
Q4: How often do electrolyte analyzers need calibration?
Modern analyzers (like the Seamaty SE1) feature automated calibration with each test cartridge, eliminating manual calibration. High-throughput systems require daily calibration to maintain precision, as recommended by ISO 13485 standards.
Future Trends in Electrolyte Testing (2026–2035)
The electrolyte analyzer market is growing at a steady CAGR, with 2026 innovations focusing on:
- Miniaturization & Portability: 35% growth in compact POCT models, making testing accessible in remote and low-resource settings.
- Cartridge-Based Testing: 24% development of cartridge systems, reducing cross-contamination and simplifying workflow.
- IoT & Connectivity: 34% integration with hospital IT systems, enabling remote performance monitoring and proactive maintenance.
- Multi-Parameter Integration: Combining electrolyte, blood gas, and metabolic testing in single devices, aligning with 28% growth in multi-parameter testing.
Conclusion
An electrolyte analyzer is an essential diagnostic tool for 2026 healthcare—supporting timely diagnosis, effective treatment, and improved patient outcomes across clinical, emergency, and POCT settings. With ISE technology as the gold standard, modern analyzers balance speed, accuracy, and convenience, addressing the diverse needs of small clinics, large hospitals, and mobile health units.
Among the 2026 options, the Seamaty SE1 Electrolyte Analyzer stands out for its portability, ease of use, and rapid results—making it an ideal choice for facilities prioritizing efficiency, cost-effectiveness, and patient-centric care. By aligning your device selection with your lab’s throughput, testing needs, and budget, you can leverage 2026’s latest innovations to optimize electrolyte testing workflows.
To explore the Seamaty SE1 and its full capabilities, visit the official product page for detailed specs, reagent options, and partnership opportunities.
Leave A Comment